We left off last time pondering the differences between modern life and the old days. Are humans simply taking in more and burning less energy than ever before? Is it only that people are eating more calories and exercising less? Is it feasible to entertain the notion that the obesity epidemic could be explained in some way that contradicts, or goes beyond, or adds to that understanding?
One of the possibilities is that contemporary life causes more stress, but we rejected that. Oppressed by a sword-wielding warlord; persecuted by a paranoid office manager; eaten by a tiger; hit by a car. Humans have always had worries and problems.
Of course, a counter-argument could be: Despite the fact that humans have always lived with stress and had to cope with it, things are different now. Some researchers believe their findings show that chemicals in the air, food, and water have affected our bodies’ ability to protect and heal, and diminished our ability to negate the effects of stress in the age-old ways.
This paragraph from Medscape states the case, and gives a list of things that have some kind of influence and impact:
The etiology of obesity is far more complex than simply an imbalance between energy intake and energy output. Although this view allows easy conceptualization of the various mechanisms involved in the development of obesity, obesity is far more than simply the result of eating too much and/or exercising too little.
Possible factors in the development of obesity include the following: Metabolic factors; genetic factors; level of activity; endocrine factors; race, sex, and age factors; ethnic and cultural factors; socioeconomic status; dietary habits; smoking cessation; pregnancy and menopause; psychological factors; history of gestational diabetes; lactation history in mothers.
Many of these conditions are materially different than they were a thousand years ago. According to an old saying, “There’s many a slip ‘twixt the cup and the lip.” In the same way, it’s becoming uncomfortably obvious that a lot of offices and laboratories are harboring mavericks who have a similar feeling about the prevalence of slips between “energy in” and “energy out.”
Russell Farris, author of The Potbelly Syndrome, describes himself thus:
I’m a retired artificial-intelligence researcher who spent most of my life solving problems for the U.S. Navy. After my heart attack in 1998, I began to apply my problem-solving experience to the study of heart disease and related illnesses.
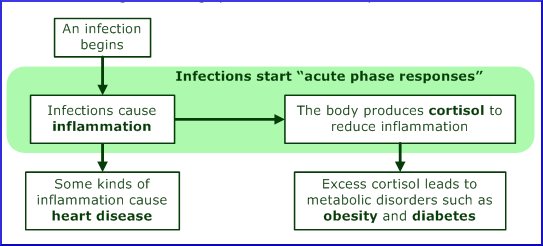
Farris proposes that we all have an infectious burden — usually, at the very minimum, chronic cases of chlamydia and herpes. In response, the body produces immune cells, cortisol, and cytokines, which cause inflammatory and metabolic disorders, resulting in “side-effects of adaptations that our bodies make to fight infections” — obesity, type 2 diabetes, and heart disease.
To doubters, he says:
Medline Plus News is a daily summary of research findings, written in plain English… There are two or three articles each week confirming the ideas presented in The Potbelly Syndrome.
When cortisol is produced to fight infection, we get chronic subtle hypercortisolism, which is, Farris says, is an extension of metabolic syndrome. He anticipates the question that any reasonable person would ask: “If all adults are infected with germs that raise their cortisol levels and make them insulin resistant, why aren’t they all fat?” And answers it:
This question stumped me until I read a book called Fight Fat After Forty by Pamela Peeke, M.D. She explains that cortisol is produced by a group of organs called the hypothalamic-pituitary-adrenal (HPA) axis. The HPA axis produces other hormones besides cortisol, and one of them is corticotropin-releasing hormone (CRH). Dr. Peeke calls CRH the ‘alarm hormone.’ She wrote: ‘The Alarm Hormone is one of the most potent appetite suppressants we know of’ (page 47). The interaction of CRH and cortisol makes some people slender and other people fat. That’s not the only reason why some people stay slim, but it’s an important reason.
But there is more:
Cortisol stimulates our appetites, and it makes fat stick to our bellies. It also makes us obese by raising our glucose and insulin levels… Cortisol has been linked to a number of addictive substances, so the U.S. National Institute on Alcohol Abuse and Alcoholism has an interest in it.
What if there is something to all this? What if it turns out that food addiction starts with too much cortisol, caused by chronic infection? Wouldn’t that be worth writing home about?
Your responses and feedback are welcome!
Source: “Etiology,” Medscape
Source: “Dysphoria & Obesity,” PotbellySyndrome.com
Image by Russell Farris.

 FAQs and Media Requests:
FAQs and Media Requests: 











