Where COVID-19 is concerned, obesity, as we have been discussing, is a huge risk factor for both adults and children. And staying home to avoid the illness is a huge risk factor for obesity. They feed off each other in a devastating partnership.
There are other interesting factoids (trivia would certainly be an inappropriate word) about the sickness to know. For example, no matter how much a patient suffers, if the blood levels can be maintained without supplemental oxygen, the case is officially categorized as “mild.”
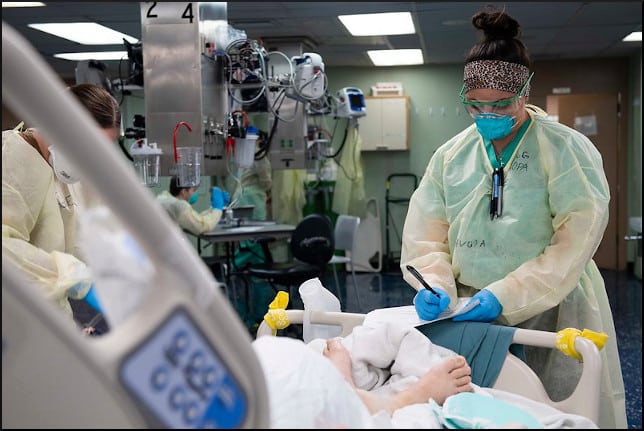
Onward, now, to the science-fictional environment where a person least wants to be. It looks like an alien abduction scenario. A 2012 study concentrated on the Intensive Care Units of 106 American hospitals, some with multiple ICUs, bringing the total to 156 units in all. But wait until you hear the number of patient records that were studied — almost 200,000.
The specific object of the quest was ICU recidivism. In other words, how many of those patients were not ready to be released, and had to return to the ICU? The number at that time was about 4% returnees, within an arbitrarily designated five days after discharge. In other words, after five days, a necessary readmission would be considered a separate incident, not a continuation of the first incident. We will see why such a detail matters.
A very significant digression
Just imagine a world where all middle-school students took a class in how to read a scientific study. Those reports are all organized the same way, and there is a method to extracting the pertinent information. Sadly, journalists often don’t. They skip over the parts they don’t care for, or put too much stress on the part they do like, and have a tendency to ignore the caveats that the researchers prudently included. Consequently, segments of the news-consuming public get strange ideas.
Also, journalists, and people with particular agendas, might do the equivalent of comparing apples to oranges. Looking at any pair or group of studies, the meta-analyst has to be really scrupulous about making sure the details match up. Say there’s another study, from Britain perhaps, of neonatal ICU facilities and how many babies are released when they are not quite ready. And those researchers define a medically dangerous release as seven days. So, already, two factors are different.
When researchers set out to do a meta-study employing data from many different studies, as a preliminary step they have to comb through the available material carefully, and probably reject a good many papers, unable to line up enough methodological similarities to validate the drawing of any conclusions.
So what?
Opinions about COVID-19 are very contentious, partly for this same reason. People compare studies that really should not be linked for informational purposes; or latch onto the title and disregard the fine print. The reluctance or inability to understand a research paper can lead to a perception that scientists are a bunch of bumbling idiots, or worse yet, that ordinary people are being lied to.
Sometimes, to learn what is really going on takes a lot of drilling down. Research typically finds not a slam-bang answer, but an incremental one, revealed over time in a frustrating dance of seven veils. In Coronavirus Land, patients who make it to the ICU typically stay hospitalized for a few weeks. This is not optimal, because practitioners need answers now. Here is a sad detail of that 2012 study:
Readmitted patients had a much higher mortality (20.7%) than first-time ICU admissions (3.7%).
The massive outbreak in the Lombardy region of Italy led to tracking of patients admitted between late February and late March. Out of 1,300 people, 1,287 (or almost all of them) needed respiratory support (intubation: 88%; non-invasive ventilation: 11%). The ICU mortality rate was 26%, or just over one-fourth.
This paragraph of a multi-author study give a sense of the limitations faced by researchers:
First, this was a retrospective study, and data were acquired via telephone. Second, the critical nature of the Lombardy situation did not allow the coordinator to obtain more detailed information, such as baseline medication use. Third, the follow-up time is still relatively short compared with the course of the disease, and the reported mortality data and length of stay data reported in this study could change. Fourth, there were relatively large amounts of missing data for some outcomes.
Because the problem is new and ongoing, most coronavirus studies are very small and necessarily inconclusive. The question of a one-year survival rate, for example, is not even broached because a year ago, nobody had the disease. In one small Seattle study, half the patients died without ever leaving the ICU. Journalist Aylin Woodward mentions another Washington State study of 21 coronavirus patients in ICU (17 of them on mechanical ventilation) where 67% died, and when the study ended 24% were still critically ill, and only two individuals had been discharged.
Your responses and feedback are welcome!
Source: “‘She’s Out of the ICU Now.’ ‘That’s a Relief, Isn’t It?”: The Growing Problem of ICU Recidivism,” ATSJournals.org, 05/01/12
Source: “Baseline Characteristics and Outcomes of 1591 Patients Infected With SARS-CoV-2 Admitted to ICUs of the Lombardy Region, Italy,” JAMANetwork.com, 04/06/20
Source: “Boris Johnson is in intensive care with COVID-19,” BusinessInsider.com, 04/07/20
Image: Public Domain

 FAQs and Media Requests:
FAQs and Media Requests: 











