Yesterday, Childhood Obesity News discussed a recent article by The Wall Street Journal‘s Melinda Beck, who mentioned that the nutritional deficiency theory of food cravings seems to be disproved, because so many cravings are addressed to food-like substances that have no provable “minimum daily requirement” to maintain human health.
On the other hand, Dr. Douglas Hunt had an answer for this back in 1988 that might still hold up. In No More Cravings, he wrote:
If only a single major mineral is missing, such as salt, the internal information feedback systems make it clear to the brain that salt will bring relief. Ample research in this area makes it undeniable that salt cravings relate to salt deficiencies. However, when there are multiple deficiencies of less clearly defined vitamins and minerals, messages to the brain are often confused. The brain cannot get a clear picture of what substance would relieve the discomfort.
This leads to all kinds of havoc. It is no coincidence that the salty snack is a major childhood obesity villain. It would not be too surprising to learn that genuine deficiency cravings for all kinds of obscure nutrients could be misinterpreted by receptors that have been bludgeoned into numbness by overuse, with the result that the overwhelmed organism just wants salt, salt, salt.
Dr. Hunt in his practice appears to have encountered the food addiction equivalent of crack babies, saying:
It may begin before birth if the mother takes in too much salt during pregnancy. Salty baby foods follow, then junk foods during childhood.
Among the researchers mentioned by Beck, who have been using functional MRI scans to visualize the effect of food cravings on the brain, is Marcia Pelchat, Ph.D., of the Monnell Center, whose list of interests illustrates how highly specialized a career can be:
1) food preferences, especially mechanisms of food cravings, responses to novel foods, and food preferences in the elderly
2) chemical senses in the elderly including taste, smell, and chemical irritation
3) genetics of individual differences in human chemosensation
4) neuroimaging of sensory and evaluative responses to food
Along with Joyce A. Corsica, Ph.D., Pelchat was the author in 2010 of “Food Addiction — True or False?” whose “Summary” (PDF) includes the words:
Screening for food addiction has the potential to identify people with eating difficulties that seriously compromise weight management efforts. Future research should include a focus on human food addiction research; evaluating the impact of treatment on underlying neurochemistry; and prevention or reversal of food addiction in humans.
Overall, it seems to be a general principle that food cravings will become weaker, the longer they can be resisted, and Beck mentions some ways that people have found to successfully fight down their urges. One is to “embrace and control” the urge. For instance, a British study indicated that if a chocoholic only ate chocolate for dessert, or even in the middle of a meal, cravings would be easier to control than if they ate chocolate on an empty stomach.
But this has little to do with serious addiction. A 12-step program would not recommend heroin on weekends only. The rule is, heroin must be out of the picture. No has to mean no. Because that’s the very nature of addiction. Control, moderation — those words are not in the addict vocabulary. For successful recovery, halfway measures just don’t work.
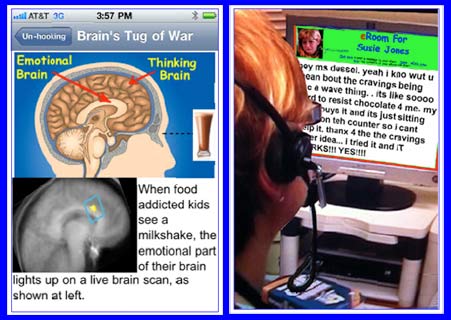
The picture on this page includes two of the many interesting illustrations from Dr. Pretlow’s presentation at the recent annual meeting of the Obesity Society. Titled “Addiction Model Intervention for Obesity Implemented as a Smartphone App: a Pilot Study,” it is available as a PDF download.
Your responses and feedback are welcome!
Source: “How to Fend Off a Food Craving,” The Wall Street of Journal, 09/17/12
Source: “Marcia Pelchat,” Monnell.org
Source: “Food Addiction — True or False?,” Google Docs, 2010

 FAQs and Media Requests:
FAQs and Media Requests: 











