We were talking about relationships between kids, their parents, and the people designated to monitor children’s health. There are certain things that should be known by every professional whose practice concerns childhood obesity — and whose does not? Especially for those who are responsible for weighing and measuring children, it’s always important to understand the basics. This need is met by Assessment of Children, by Barbara J. Moore, Ph.D., a well-thought-out tutorial for professionals.
Available as a PDF file, the handbook was compiled by the president and CEO of Shape Up America! and its purpose is to aid in the assessment and prevention of obesity in children. It sets up, in a most emphatic way, the expectations:
Children should be measured in a respectful manner in a confidential and private setting. The data should be treated with the utmost care to insure confidentiality and should be shared with parents/caregivers as specified by locally applicable laws, policies or regulations.
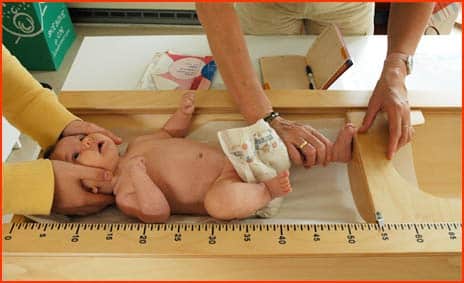
There are complete instructions for the correct method of measuring body mass index (BMI) including some that make it clear how differently the procedure fits into a routine doctor visit and the environment of a public school where a great number of individuals have to be accommodated. The setting should of course be private, and the child should be weighed in light clothing only, without shoes or socks (although socks might need to be left on for “practical purposes”). In fact, the text goes on to specify that for the measurement of height, there should absolutely be no socks.
Weighing should be done before a meal, a circumstance which parents need to be aware of when bringing kids to a doctor or clinic, and which might be hard to manage in a public school setting, where there are many scheduling factors to take into consideration. Also, weight should be taken “after voiding,” which suggests what might, to some parents, be troubling questions. Can public schools really order children to use the bathroom on command? How much disrobing can be done to achieve the “light clothing only” stricture, before someone objects and starts talking about legal action?
Among other resources, Assessment of Children offers form letters that can be adapted to the particular practice or institution. There are letters for notification of Normal Weight Status, Overweight Status, Obesity Status, Underweight Status, and for opting out.
Dr. Moore devotes much attention to the initiation of interventions with parents, listing several of the potential problems, starting with the fact that many parents are truly oblivious to the overweight condition of their own children. They console themselves with the “big-boned” cliché, or convince themselves that kids will grow out of a chubby stage (which is sometimes true and perfectly natural.)
If other health care professionals in the child’s life have not previously raised a red flag, parents will be increasingly unwilling to believe each successive professional, on the grounds that if anything was wrong, somebody else would have mentioned it already. Although it’s hard to believe in these over-communicative days, some parents are not even aware of the medically serious and even life-threatening implications of childhood obesity.
And even if parents recognize a problem and are willing to take the necessary steps, sometimes they just don’t know what to do. In the average family, there are already plenty of issues going on between parents and children. If the family situation is already tense, they don’t want to make it worse. If the home atmosphere is relatively sane and peaceful, nobody wants to rock the boat.
Still, the booklet advises, once the parents acknowledge a problem and are psychologically ready to take action, they will want suggestions and recommendations, and the health care professional had better be prepared. Here is a sample:
Children typically want direct messages, small attainable goals, and parental support and acceptance.
To help their overweight children, parents are advised to:
• Communicate that their child is loved and accepted as they are today.
• Make family changes in lifestyle rather than impose individual changes on the child.
• Consult with the family health care provider before initiating dietary changes.
Your responses and feedback are welcome!
Source: “Assessment of Children” (PDF), ShapeUp.org
Image by Tom & Katrien, used under its Creative Commons license.

 FAQs and Media Requests:
FAQs and Media Requests: 











