 In “Weight Loss Surgery, Part 4,” we looked at the experiences of some grownups with bariatric surgery. But what about the kids? Is weight loss surgery (WLS) recommended for obese children and youth? Dr. Laurie Barclay discussed this for Medscape not long ago, summarizing research that had been reported in the medical journal Clinical Obesity. She quotes lead author Andrea Aikenhead from the International Association for the Study of Obesity, who said in a news release, “The obesity epidemic now affects children as well as adults, with obesity and its associated morbidities and costs increasing in scale.”
In “Weight Loss Surgery, Part 4,” we looked at the experiences of some grownups with bariatric surgery. But what about the kids? Is weight loss surgery (WLS) recommended for obese children and youth? Dr. Laurie Barclay discussed this for Medscape not long ago, summarizing research that had been reported in the medical journal Clinical Obesity. She quotes lead author Andrea Aikenhead from the International Association for the Study of Obesity, who said in a news release, “The obesity epidemic now affects children as well as adults, with obesity and its associated morbidities and costs increasing in scale.”
It was one of those meta-studies, based on all-known research on a topic within certain parameters. In this case, they wanted histories for patients under 19 years of age, “with 1 or more measurements of postoperative weight loss and at least 1 year of postoperative follow-up.” They looked at 37 studies in all, encompassing young veterans of gastric banding, Roux-en-Y gastric bypass, sleeve gastrectomy, biliopancreatic diversion, and the now unpopular vertical banded gastroplasty.
They gleaned an awful lot of information, including the finding by a pragmatic Australian research team which concluded that “laparoscopic adjustable gastric banding (LAGB) is cost effective for adolescents.” Some of the most interesting material is on post-op problems. Aside from three surgery-related deaths, Barclay says,
Various surgical procedures were associated with a range of postoperative complications including ulcers, intestinal leakage, wound infection, anastomotic stricture, nutritional deficiencies, bowel obstruction, pulmonary embolism, disrupted staple lines, band slippage, psychological sequelae, and repeated vomiting.
For older kids, bariatric surgery can help them lose weight and alleviate the life-threatening medical conditions associated with obesity. But the evidence suggests that teens are less adept than adults at following orders, even important ones having to do with post-surgical follow-up and subsequent self-disciplined behavior. No surprise there. Adolescents are not famous for their compliance in any realm of life.
The study authors do worry that not enough data are available to really get a good handle on long-term results. If surgery has to be done on children at all, they recommend the reversible kind, and an extremely cautious approach. They are also very frank about the shortcomings of this type of research, which Barclay describes below:
Limitations of this study include retrospective or observational design in most studies, insufficient power, generally small sample sizes, results not broadly comparable, and limited information for low-frequency outcomes such as mortality and complications. In addition, it was difficult to determine the degree of weight regain in adolescents, in part because of the bias introduced by patients lost to follow-up.
The study authors feel there is an immediate need to develop other ways than surgery to treat childhood obesity. They vaguely recommend “practical lifestyle programs that are effective, even modestly, for overweight and obese children.”
Dr. Robert A. Pretlow, as we know, recommends recognizing the obesity epidemic for the addiction problem it is, and finding a way to get kids into residential addiction recovery programs that address the root of their dependency issues. In other words, something that has a real chance of working long-term.
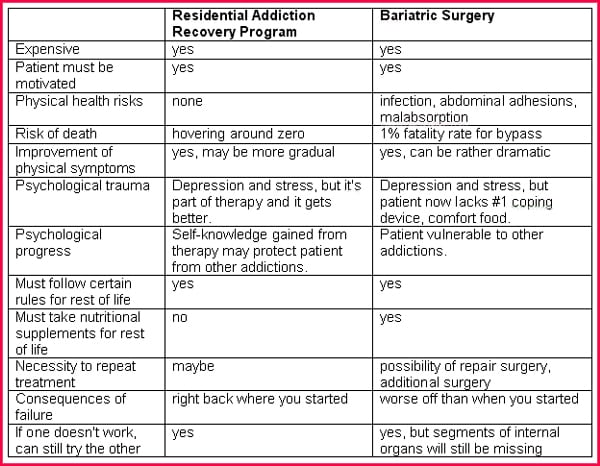
The Childhood Obesity News Comparison Chart
Your responses and feedback are welcome!
Source: “Bariatric Surgery May Be Helpful in Pediatric Population,” Medscape, 03/15/11
Image by colros (Sandra Cohen-Rose and Colin Rose), used under its Creative Commons license.

 FAQs and Media Requests:
FAQs and Media Requests: 












One Response
I have a niece who lost weight easily using supplements.